AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
We used stata 13.0 statacorp lp usa4/30/2024 There continues to be a paucity of recent large studies exploring temporal trends in the use of ERCP. Some of the key factors that have been noted to influence competency positively include training at large-volume centers and a bile duct cannulation rate of 80 % to 90 %, emphasizing that the total number of procedures to achieve proficiency varies among trainees and should, as such, be individualizedĪlthough previous epidemiological data are available on the topic, there have been significant recent technological and scientific advances in advanced endoscopy. As the demand for advanced endoscopists continues to increase, the number of academic programs offering ERCP training has increased, which highlights the importance of competency assessment in the area During that final year, the trainee is expected to acquire the necessary cognitive skills for decision-making, as well as the core ERCP technical skills In the United States, current training in ERCP requires a prior 3-year training in internal medicine followed by a 3-year training program in general gastroenterology and finally an additional year in advanced endoscopy training. Previous reports have shown that inpatient utilization of ERCP has been decreasing since 1996, which is believed to be due to the widespread availability of newer imaging modalities such as magnetic resonance cholangiopancreatography (MRCP) and endoscopic ultrasound (EUS) In recent years, the role of ERCP has shifted from being a diagnostic and therapeutic procedure, to mainly being a therapeutic procedure ERCP was initially developed in the late 1960’s as a diagnostic procedure and subsequently evolved to a therapeutic procedure with the first biliary sphincterotomy performed in 1974 in Kyoto, Japan These findings may reflect the increased case complexity and fact that ERCP continues to evolve into an increasingly interventional tool, contrasting from its former role as a predominantly diagnostic and gallstone extraction tool.Įndoscopic retrograde cholangiopancreatography (ERCP) is a complex endoscopic procedure used to evaluate pancreatobiliary ductal anatomy through the use of fluoroscopy and contrast to determine suitable interventions for both benign and malignant pathology. 
Hence, physicians must be aware to promptly diagnose and treat complications. The most common principal diagnoses were choledocholithiasis and gallstone-related AP. Odds of therapeutic interventions and complications increased. The number of ERCPs increased in the past decade. Hospital charges increased, while length of stay (LOS) decreased. Patients undergoing ERCP in 2016 had greater odds of undergoing bile duct stent placement, pancreatic duct (PD) stenting, biliary dilation, pancreatic sphincterotomy, PEP and biliary perforation. The total number of ERCPs increased over the last decade.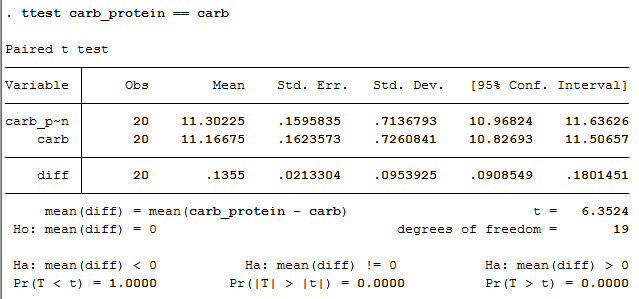 
Multivariate regression analysis was used to adjust for confounders.Ī total of 1,606,850 patients underwent inpatient ERCP. Secondary outcomes included determining procedural specifics (stenting, sphincterotomy and dilation), complications (post-ERCP pancreatitis, bile duct perforation), hospital length of stay, total hospital costs and charges. 
All patients with ICD9–10CM procedural codes for ERCP were included. Retrospective-cohort study using the Nationwide Inpatient Sample 2007–2016. Thus, the aim of this study was to assess the inpatient use of ERCP, outcomes, and most common indications. Despite advances in ERCP, paucity in recent literature regarding utilization and outcomes of ERCP exists. With newer imaging modalities, indications for use of endoscopic retrograde cholangiopancreatography (ERCP) have changed in the last decade.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
